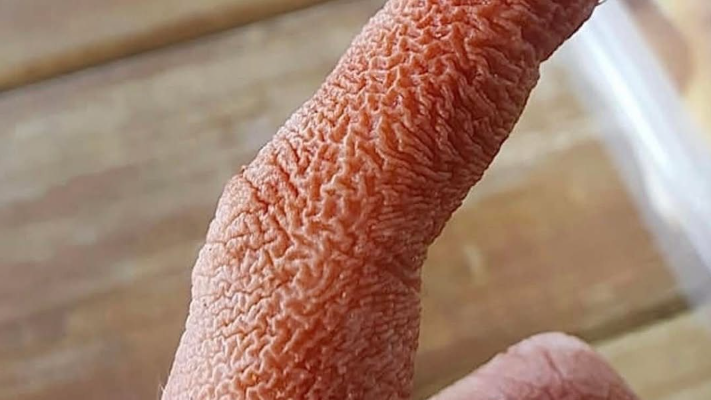
Clinical Presentation
The most striking feature in the image is marked xerosis, which is the medical term for abnormally dry skin. The skin appears rough, with deep lines and a cracked texture, suggesting a compromised skin barrier. In many cases, this kind of presentation may be linked to conditions such as eczema, also known as atopic dermatitis, or chronic irritant contact dermatitis.
Patients with severe xerosis or eczema often present with:
- Dry, scaly skin that may feel tight or rough
- Hyperkeratosis, where the outer layer of skin becomes thickened
- Fissures or cracks, which can sometimes be painful or bleed
- Itching (pruritus), which may lead to scratching and further skin damage
- Redness or inflammation, although in chronic stages the skin may appear more leathery than inflamed
In the case shown, the absence of obvious redness suggests a more chronic phase rather than an acute inflammatory flare. The exaggerated wrinkling could also indicate repeated exposure to water, chemicals, or environmental irritants that have stripped the skin of its natural oils.
Another possible contributor is occupational exposure. Individuals who frequently wash their hands, handle cleaning agents, or work in environments with low humidity often develop this kind of skin change. Healthcare workers, cleaners, and food handlers are particularly at risk.
Differential Diagnosis
While eczema is a leading possibility, other conditions should also be considered:
- Contact dermatitis: Caused by repeated exposure to irritants like soaps, detergents, or solvents
- Psoriasis: Typically presents with thicker plaques and silvery scales, but can sometimes resemble severe dryness
- Ichthyosis vulgaris: A genetic condition characterized by widespread dry, scaly skin
- Dehydration or environmental factors: Cold weather, low humidity, and excessive handwashing can all contribute
A proper diagnosis would depend on clinical history, including symptom duration, occupational exposure, and any associated itching or pain.
Pathophysiology
At the core of this condition is a disruption of the skin barrier. The outermost layer of the skin, known as the stratum corneum, is responsible for retaining moisture and protecting against external irritants. When this barrier is compromised:
- Water is lost more rapidly from the skin (transepidermal water loss)
- The skin becomes dry, cracked, and more susceptible to irritation
- Inflammatory pathways may be triggered, especially in eczema
Repeated washing, harsh soaps, and environmental exposure can strip away natural lipids, worsening the condition over time.
Management
Effective management focuses on restoring the skin barrier, reducing irritation, and preventing recurrence.
1. Moisturization
The cornerstone of treatment is regular and intensive use of moisturizers. Products containing:
- Urea
- Glycerin
- Ceramides
- Petrolatum
are particularly effective. These ingredients help attract moisture and lock it into the skin. Thick creams or ointments are generally better than lotions.
Moisturizers should be applied:
- Immediately after washing hands
- Multiple times throughout the day
- Before bedtime, possibly with cotton gloves to enhance absorption
2. Avoidance of Irritants
Identifying and minimizing exposure to irritants is crucial. This includes:
- Switching to mild, fragrance-free soaps
- Avoiding hot water; using lukewarm water instead
- Wearing protective gloves when handling chemicals or cleaning agents
However, prolonged glove use without ventilation can also trap moisture and worsen skin breakdown, so balance is important.
3. Topical Medications
If inflammation or itching is present, topical corticosteroids may be prescribed to reduce inflammation. These should be used under medical guidance to avoid side effects such as skin thinning.
In some cases, topical calcineurin inhibitors (like tacrolimus) may be used, especially for chronic eczema.
4. Hydration and Environmental Control
Maintaining adequate hydration and improving environmental conditions can also help:
- Use a humidifier in dry indoor environments
- Drink sufficient water
- Avoid extreme cold or dry air when possible
5. Advanced Therapies
For severe or persistent cases, referral to a dermatologist may be necessary. Treatments could include:
- Prescription-strength barrier repair creams
- Phototherapy (light therapy)
- Systemic medications in rare, severe cases
Prognosis
With proper care, most cases of severe dryness or eczema can be significantly improved. However, chronic conditions may require ongoing maintenance. Without treatment, the skin can continue to crack, increasing the risk of infection and discomfort.
When to Seek Medical Attention
Medical evaluation is recommended if:
- The skin becomes painful, swollen, or infected
- There is no improvement with over-the-counter treatments
- Symptoms interfere with daily activities
Conclusion
The finger in the image demonstrates a classic example of severe skin dryness with likely chronic irritation or eczema-related changes. While the appearance can be alarming, the condition is usually manageable with consistent skincare, avoidance of irritants, and appropriate medical treatment when necessary.
The key takeaway is that skin barrier repair and protection are central to both treatment and prevention. With the right approach, even significantly affected skin can regain much of its normal texture and function over time.